Medical Needs

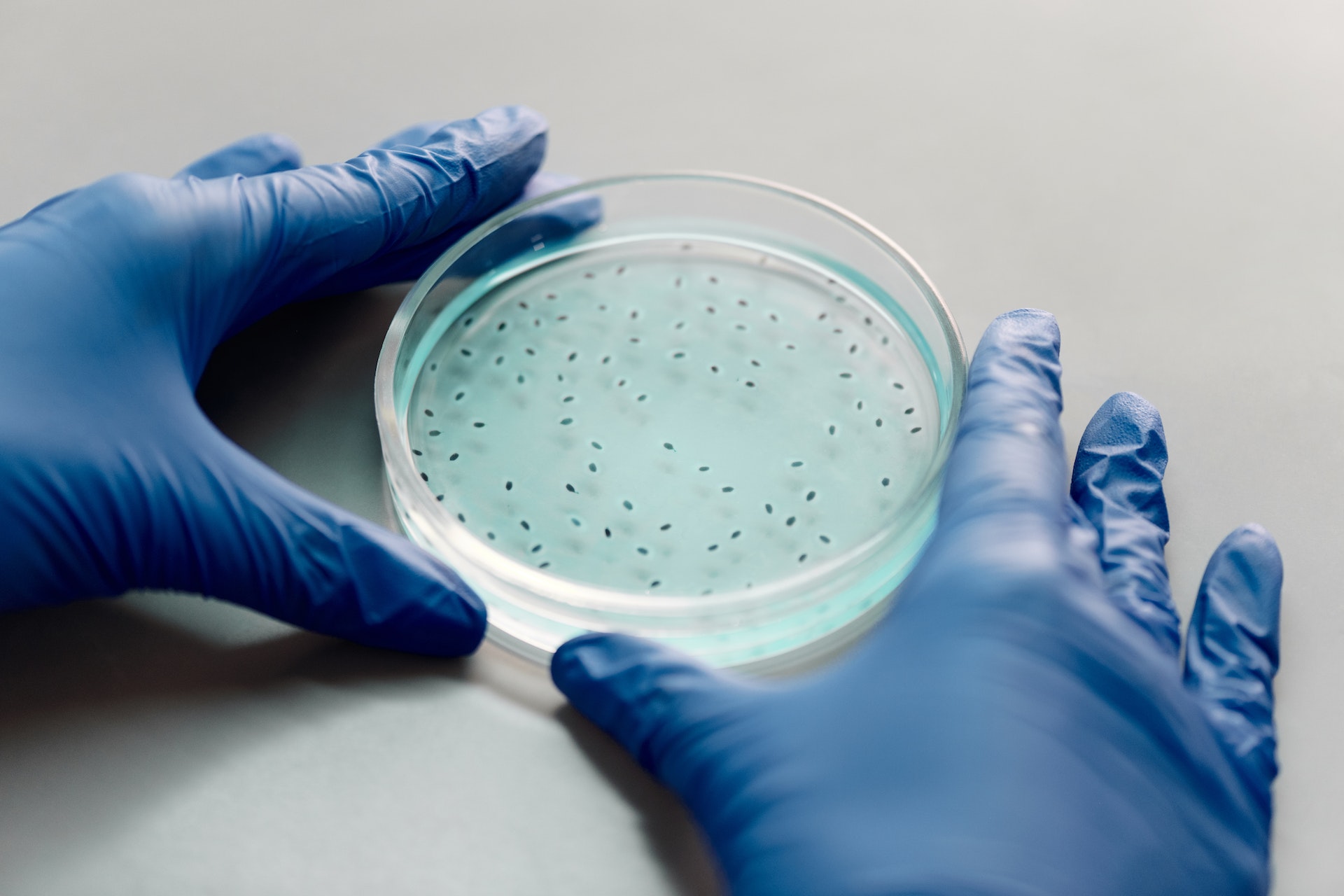
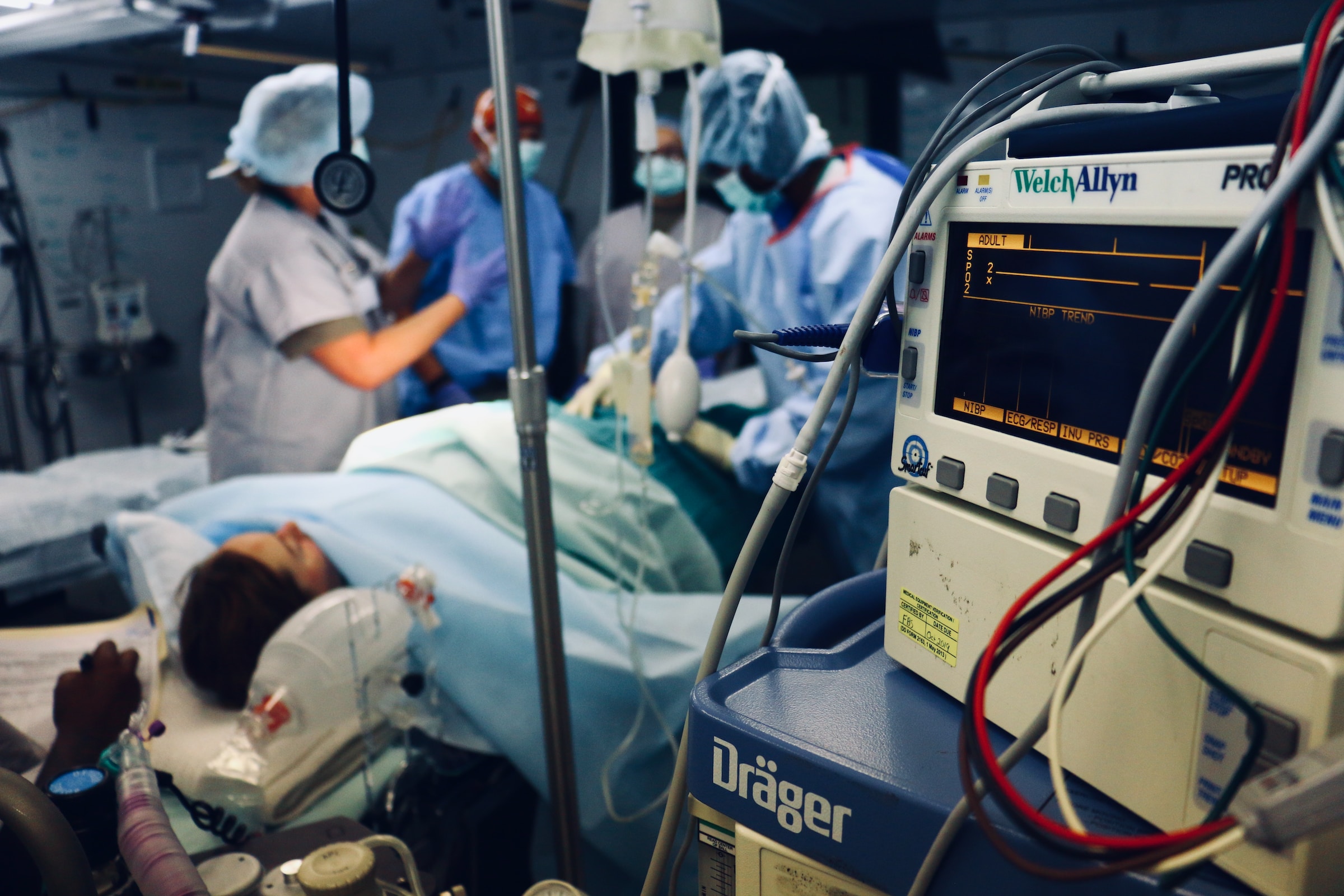
Hospital-acquired infections (HAIs), also known as nosocomial infections, are infections that develop in patients when they receive medical care in a healthcare facility (hospital, clinic or nursing home). Globally, hundreds of millions of people every year are affected by Hospital-acquired infections (HAIs) and no country or health system, even the most developed or sophisticated, can claim to be free of HAIs. HAIs are mainly acquired in intensive care units (ICUs), neonatal units and after surgery. Up to 30% of patients are affected by a least one HAI in ICUs while this rate is 3-20 times higher in neonatal units.
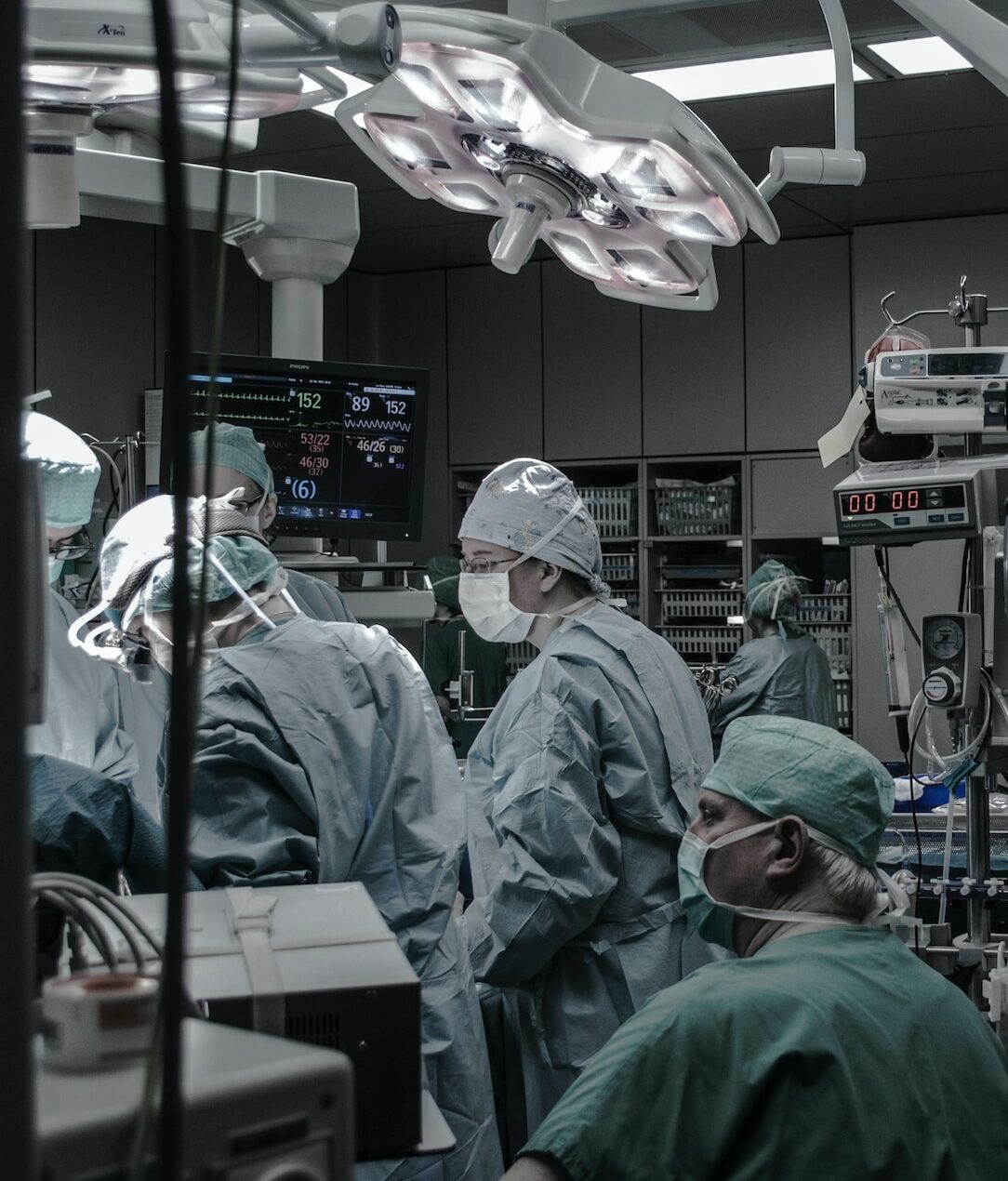
The Centers for Disease Control and Prevention (CDC) has estimated that every day in the US, 1 in 31 hospitalized patients has an HAI which leads to direct medical costs of at least $28.4 billion each year2. In Europe, according to the European Centre for Disease Prevention and Control (ECDC), of the 120,446 patients staying more than two days in an intensive care unit in 2019, 8,874 contracted HAIs.
Today, the health emergency linked to HAIs results from the emergence of antibiotic-resistant bacteria. Indeed, healthcare establishments are often environments where patients are exposed to antibiotic treatments whose excessive and inappropriate use can promote the development and transmission of resistant bacteria within the hospital population.
In a study conducted between 2012 and 2017 in the United States, out of a cohort of 41.6 million hospitalizations, 622,390 patients had contracted an infection caused by multidrug-resistant bacteria, 17% of which occurred in hospital. A similar study was carried out in China between 2012 and 2014 and revealed that out of a sample of 15,588 patients, 7,579 had contracted HAIs, of which 3,223 were due to MDR bacteria.
Despite advances in the understanding of contributing causes and prevention, Healthcare-Associated Pneumonia (HAP/VAP) continue to be frequent complications of hospital care. Together, they are among the most common hospital-acquired infections (HAIs), accounting for 22% of all HAIs in a multistate point-prevalence survey conducted in the US.
As with any type of infection, HAIs can cause sepsis, particularly in people who are already at risk, such as those with chronic illnesses, who are immunocompromised, the very young, and the very old.